What is skin cancer?
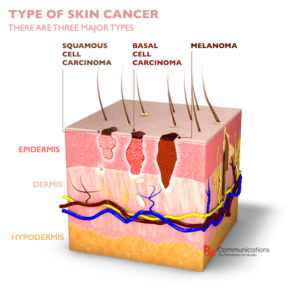
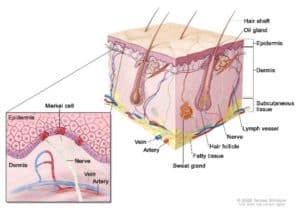
Skin cancer occurs when there is out-of-control growth of mutated, abnormal cells in the outermost layer of skin, called the epidermis. It is caused by unrepaired DNA damage that causes cell mutations. Due to these mutations, the skin cells multiply rapidly and form malignant tumours.
The main types of skin cancer that can occur are melanoma, squamous cell carcinoma (SCC), Merkel cell carcinoma (MCC) and basal cell carcinoma (BCC).
The two leading causes of skin cancer are harmful ultraviolet (UV) rays from the sun and the extensive use of tanning beds which also use concentrated UV radiation. The good news, however, is that if you can catch skin cancer early a dermatologist will be able to treat it with minimal or no scarring and a high likelihood that it will be removed entirely.
In a lot of cases, the growth may be caught before it reaches the cancerous stage so that it does not become skin cancer or penetrates below the surface of the skin.
Types of skin cancer

Melanoma
What is melanoma?
Melanoma is the name of the cancer that develops from melanocytes. Melanocytes are the skin cells that produce melanin which is the pigment that gives skin its colour. According to Cancer Research UK, there were 16,700 new cases of melanoma in the UK for the years 2016-2018 (Cancer Research UK, 2021).
What causes melanoma?
Melanoma is usually caused by intense sun exposure that causes sunburns, over a long period. Tanning beds which are commonly used by people with lighter skin also increase the risk of developing melanoma.
How to check for melanoma?
Melanoma usually manifests in the form of moles or can arise through them. They are found on any part of your body, even in areas that are not exposed to the sun often. If you notice a new mole, or one that has increased in size, or is bleeding it could be a sign of potential melanoma.
Is melanoma serious?
Unfortunately, melanoma is the most dangerous of the three most common forms of skin cancer. Melanoma is the 5th most common cancer in the UK. It accounts for 4% of all new cancer cases. If they are caught early, they can often be treated and eliminated, so it makes sense to ensure you are getting regular screening to stay ahead of any potential complications.
Increased risk of melanoma
The ability to understand the causes of melanoma and if you are at higher risk of it helps you detect it early when it can be easier to treat or prevent it entirely. These factors may increase your risk of melanoma:
- Excessive and unprotected UV exposure from sun or tanning machines
- Weakened immune system
- Having pale/fair skin, light eyes or blonde/red hair
- Many moles on your body, especially if they are larger ones
- Skin cancer in family history
Things to look out for:
To find melanoma at its earliest stage there are a few things you can look out for (Skin Cancer Foundation, 2021). If you notice any changes in the following, see a dermatologist as soon as you can:
Asymmetry: Most melanomas are not even, so if you were to draw a line through the middle, both sides would not match.
Edge: Moles that may be melanoma tend to have a different edge to usual moles. They may be notched or jagged compared to the usual smooth edge of a common mole.
Colour: Common or benign moles are usually uniform in colour – they have one shade of brown. Melanoma may have a mix of colours including brown, tan or even black.
Evolution: Any change in size, colour, or shape, as well as a sudden appearance of a new mole, could be indicative of melanoma.
Bleeding: If an existing mole begins to bleed on minimal trauma, it can be a sign of malignant transformation.
It is recommended to check your skin when you can to spot these potential abnormalities and see your dermatologist for a professional examination.
Squamous Cell Carcinoma (SCC)
What is Squamous Cell Carcinoma?
SCC is the uncontrolled growth of mutated cells coming from the squamous cells in the epidermis. It is the second most common type of skin cancer (Skin Cancer Foundation, 2021a, Nazario, 2020).
What causes Squamous Cell Carcinoma?
Similarly to melanomas, SCC is caused by long-term exposure to the UV rays from the sun.
How to check for Squamous Cell Carcinoma?
SCCs can manifest as red patches, rough, thick skin, or open sores. They may have itching or bleeding and mostly occur in areas of the body that are exposed to the sun.
Is Squamous Cell Carcinoma serious?
Most of SCCs can be treated successfully if they are caught early. If not, they may form lesions that are unsightly and dangerous. They may grow into the deeper layers of your skin and even spread to more parts of your body.
Increased risk
Much of the same factors as melanoma may make you more at risk of developing squamous cell carcinoma. However, there are a few extra things that increase the risk. This includes:
- Age – if you are 50 or older you are more likely to develop SCC.
- Gender – men are more likely to develop SCC.
- Pre-existing skin conditions – if you have chronic infections or skin inflammations you may be more susceptible to developing squamous cell carcinoma.
- History of Human Papilloma Virus (HPV).
Merkel Cell Carcinoma (MCC)
What is Merkel Cell Carcinoma?
MCC is a rare form of skin cancer. It is very aggressive and is known for its high risk of returning and spreading to other parts of the body, usually within 2-3 years from the initial diagnosis.
What causes Merkel Cell Carcinoma?
This skin cancer is usually associated with the Merkel cell polyomavirus.
How to check for Merkel Cell Carcinoma?
MCC tumours most often appear on sun-exposed body areas. They aren’t very distinctive from other skin cancers and appear as pimple-type lumps. They can be skin coloured or a red/purple colour. They aren’t tender and the only thing that makes people pay attention is the speed at which they grow.
Is Merkel Cell Carcinoma serious?
This cancer has a higher risk of metastasising and recurring. As aggressive and rare as it is, it can still be treated well if caught early enough. Therefore, it is recommended to have regular skin screenings done with your dermatologist.
Increased risk
The risks of developing MCC are the same as melanoma or squamous cell carcinoma but adding to that the Merkel cell polyomavirus.
Basal Cell Carcinoma (BCC)
What is Basal Cell Carcinoma?
BCC are the most common type of non-melanoma skin cancer. They form from abnormal and uncontrolled growth from the skin’s basal cells that are also found in the epidermis (Gardner, 2020).
What causes Basal Cell Carcinoma?
The causes for BCC are the same as the other cancers. Intense sun exposure over a long period is the leading cause of basal cell carcinoma.
How to check for Basal Cell Carcinoma?
BCC usually forms in the most sun-exposed areas of the body – face, neck, scalp and back. It can appear as a small pink or white lump with a waxy appearance or like a red scaly patch.
Is Basal Cell Carcinoma serious?
BCC is the most common form of skin cancer, and in the US alone there are about 3.6 million cases found each year. In the UK basal cell carcinoma accounts for around 75 in every 100 skin cancers. It is not malignant per se in that it does not spread to distant organs in the body but if left untreated it will cause local invasion.
Increased risk
Just like the other non-melanoma cancers, increased risk factors for developing BCC is due to family history, fair/pale skin, a lot of moles and freckles and weakened immune system.
According to Cancer Research UK, there are nearly 156,000 new non-melanoma (SCC, MCC, BCC) skin cancer cases recorded in the UK each year. Of those, 47% are recorded in people aged 75 and over. Over the last decade, non-melanoma skin cancer rates have increased by 56% (Cancer Research UK, 2021a).
Skin colour and skin cancer
People who do not have light or pale skin produce more melanin in their bodies. The level of melanin production of an individual is used to be closely linked to geographical location. This is because the close you are to the equator, the more sun radiation you are exposed to. People with dark skin produce more melanin to protect themselves against UV rays.
In recent times as people have become more mobile, and technology has improved humans have moved away from their ancestral homes and as a result skin colour is not as linked to geography as it once was (Jablonski, 2012).
As a result, this has reformed the medical view that people of colour suffer less from skin cancer. The simple fact is if you have skin, you have the chance to develop skin cancer. People of colour are often diagnosed too late which makes it harder to treat.
People with dark skin who develop melanoma have around a five-year survival rate of 67% compared to 97% for people with fair skin. In the last 20 years, melanoma cases have increased by 20% among Hispanic people. SCC is the most common skin cancer among black people (Gloster and Neal, 2006).
It is important to get to know your skin type and continue to check your skin regularly regardless of skin colour.
Prevention of skin cancer
Skin cancer is the most common form of cancer in the UK, and it is the most preventable too. Protecting your skin during the first 18 years of your life can reduce your risk of some skin cancers by almost 78% (Prevent Cancer Foundation, 2021).
There are several things you can do to prevent skin cancer (British Skin foundation, 2021). This includes:
- Avoid the sun during peak hours: Avoid going out too much during summer between 10 am and 4 pm. This is when the UV rays are strongest and can cause the most damage.
- Stay in the shade: If you are outside, minimise your exposure to the sun by staying more in shady areas.
- Use sunscreen: Use a cream that covers a huge spectrum, including UVA and UVB rays. Minimum SPF level should be 15 but aim for 30 or 50 for better protection. Also, use it even on cloudy or rainy days and remember to re-apply it every few hours if you are outside.
- Wear protective clothing: When appropriate wear hats, scarves, gloves, and long sleeve shirts to reduce the amount of skin that is exposed to the sun.
- Avoid indoor tanning: Don’t use tanning beds as they expose your skin to intense UV rays and what you call a ‘base tan’ is skin damage.
- Check your skin regularly: Check any moles, freckles or birthmarks that you have. Also, check your body for any changes or abnormalities regularly and report any concerns to your doctor or dermatologist.
Echelon Health And Preventing Skin Cancer
Echelon Health aims to protect your most valuable asset. We know that there is no ‘one size fits all’ approach when it comes to everyone and their unique circumstances. Read our testimonials to learn how we adapt to help each of our clients and their individual needs.
We work together with The Mole Clinic, an award-winning, dermatologist-led skin lesion clinic. Their specialist nurses, consultant dermatologists and plastic surgeons deliver high-quality clinical care to 40,000 patients every year.
As a result, we offer a wide range of options for different scans and packages. This includes our Bespoke package which is arranged with the individual based on what they are interested in. It can include the Full Body Mole Screen where a specialist nurse will identify any visually atypical moles.
If you are interested in a fully comprehensive head-to-toe check, we have the Platinum Assessment which is one of the most comprehensive in the world. It can detect up to 92% and 95% of causes of premature deaths in males and females respectively and utilises the most advanced imaging technologies including MRI, CT scan and Ultrasound which leaves no stone unturned.
Contact us or download our brochure for more information!
Article reviewed by Paul Jenkins MA MD FRCP.
Sources:
Cancer Research UK (2021). Melanoma skin cancer statistics. Available at: https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/melanoma-skin-cancer#heading-Zero (Accessed 19/10/2021).
Skin Cancer Foundation (2021). Melanoma Warning Signs. Available at: https://www.skincancer.org/skin-cancer-information/melanoma/melanoma-warning-signs-and-images/#abcde (Accessed 19/10/2021).
Skin Cancer Foundation (2021)a. Squamous Cell Carcinoma Overview. Available at: https://www.skincancer.org/skin-cancer-information/squamous-cell-carcinoma/ (Accessed 19/10/2021).
Nazario, B. MD (2020). Squamour Cell Carcinoma. Available at: https://www.webmd.com/melanoma-skin-cancer/melanoma-guide/squamous-cell-carcinoma#1 (Accessed 19/10/2021).
Gardner, S. S. MD (2020). Basal Cell Carcinoma. Available at: https://www.webmd.com/melanoma-skin-cancer/melanoma-guide/basal-cell-carcinoma#3-8 (Accessed 19/10/2021).
Cancer Research UK (2021)a. Non Melanoma skin cancer statistics. Available at: https://www.cancerresearchuk.org/health-professional/cancer-statistics/statistics-by-cancer-type/non-melanoma-skin-cancer#heading-Zero (Accessed 19/10/2021).
Jablonski, N. G. (2012). Living color. University of California press.
Gloster HM Jr, Neal K. (2006). Skin cancer in skin of color. J Am Acad Dermatol.
British Skin Foundation (2021). Are you at risk of skin cancer? Available at: https://www.britishskinfoundation.org.uk/are-you-at-risk-of-skin-cancer#:~:text=Skin%20cancer%20is%20the%20most,that’s%20seven%20people%20every%20day (Accessed 19/10/2021).
Prevent Cancer Foundation (2021). Skin cancer. Available at: https://www.preventcancer.org/education/preventable-cancers/skin-cancer/ (Accessed 19/10/2021).